2024-05-13T10:01:00
(BPT) – By Kenji Inaba, MD, FACS, FRCSC
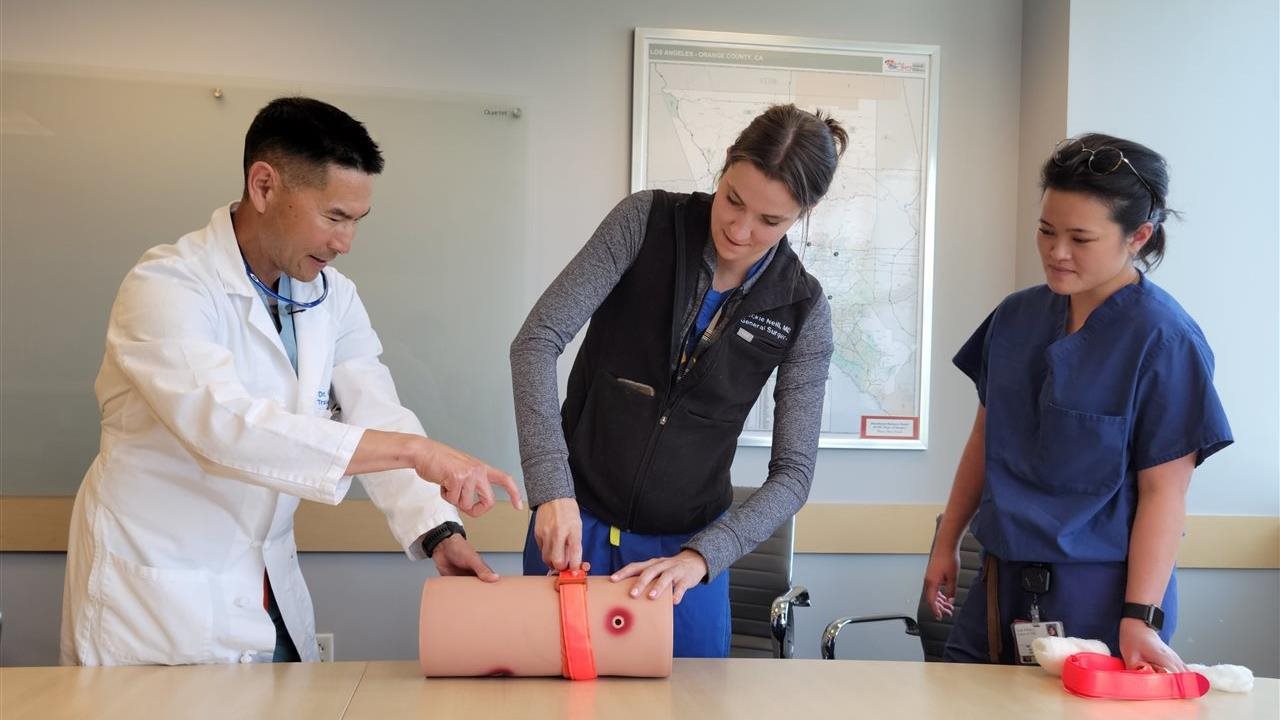
You’re on your way to work when a car crash happens. A backyard bonfire takes a turn while chopping firewood. While in your backyard, a neighbor has an accident with a lawnmower. These scenarios share a common thread — a person in need of help due to severe bleeding. This is where the American College of Surgeons Stop the Bleed® program comes in. Stop the Bleed is a simple set of skills that empowers everyday people to save lives in critical moments by learning a few basic techniques.
Training That Empowers All
May is National Stop the Bleed month and training is for everyone — parents, students, office workers, teachers — literally everyone. No background in health care is needed to get trained. Before helping, ensure your own safety and that 911 has been called. The techniques can be distilled into three lifesaving steps:
- Apply Direct Pressure: The first and most immediate step involves applying firm pressure directly to the wound, which helps to control bleeding.
- Pack the Wound: If direct pressure alone is not enough, packing the wound with gauze or a cloth can help control more severe bleeding.
- Apply a Tourniquet: For severe limb bleeding that does not stop with direct pressure or packing, a tourniquet may be necessary. This method is highly effective in stopping blood flow to a limb, thereby preventing further blood loss.
These steps form the core of Stop the Bleed training, which takes about an hour to complete — less time than it takes to watch a movie. The training is available in a variety of formats, including in-person and online options.
Originally launched in 2015, the Stop the Bleed initiative is driven by a clear vision: to equip ordinary people with the skills to prevent death from bleeding. Since then, nearly 4 million individuals globally have learned these essential skills through the program.
The Urgency of Early Action
With any injury that causes severe bleeding, the first few minutes are critical and can mean the difference between life and death. As a trauma surgeon, I have witnessed the profound impact of immediate bleeding control, observing firsthand how quick actions by bystanders can save lives. Conversely, I’ve also seen the tragic outcomes when help arrives too late.
A Call to Action
As we observe National Stop the Bleed Month in May, it’s a timely reminder of the critical importance of being prepared. Whether you’re attending a neighborhood barbecue, enjoying a day at the park, or simply going about your daily routine, the skills you learn from Stop the Bleed can prepare you to act quickly and confidently in an emergency. Lives are saved not just by the actions of medical professionals, but also by ordinary people who make extraordinary decisions to help others in need.
To join a course and buy a Stop the Bleed kit, visit stopthebleed.org.
Kenji Inaba, MD, FACS, is the Chair of the Stop the Bleed® Committee of the American College of Surgeons Committee on Trauma, Chief of Trauma at the Los Angeles General Medical Center, and a Professor of Surgery at the University of Southern California.