2024-02-12T11:01:00
(BPT) – Did you know that the heart beats about 70 times per minute?1 Despite this muscle only being about the size of your fist, it is responsible for pumping oxygen-rich blood throughout your entire body 24/7 using arteries or blood vessels.1
When there is a narrowing or blockage of the coronary arteries due to a build-up of plaque, it can threaten the supply of oxygen and blood to the heart.1 This can result in a condition known as coronary artery disease (CAD), which is the most common type of heart disease in the United States.1
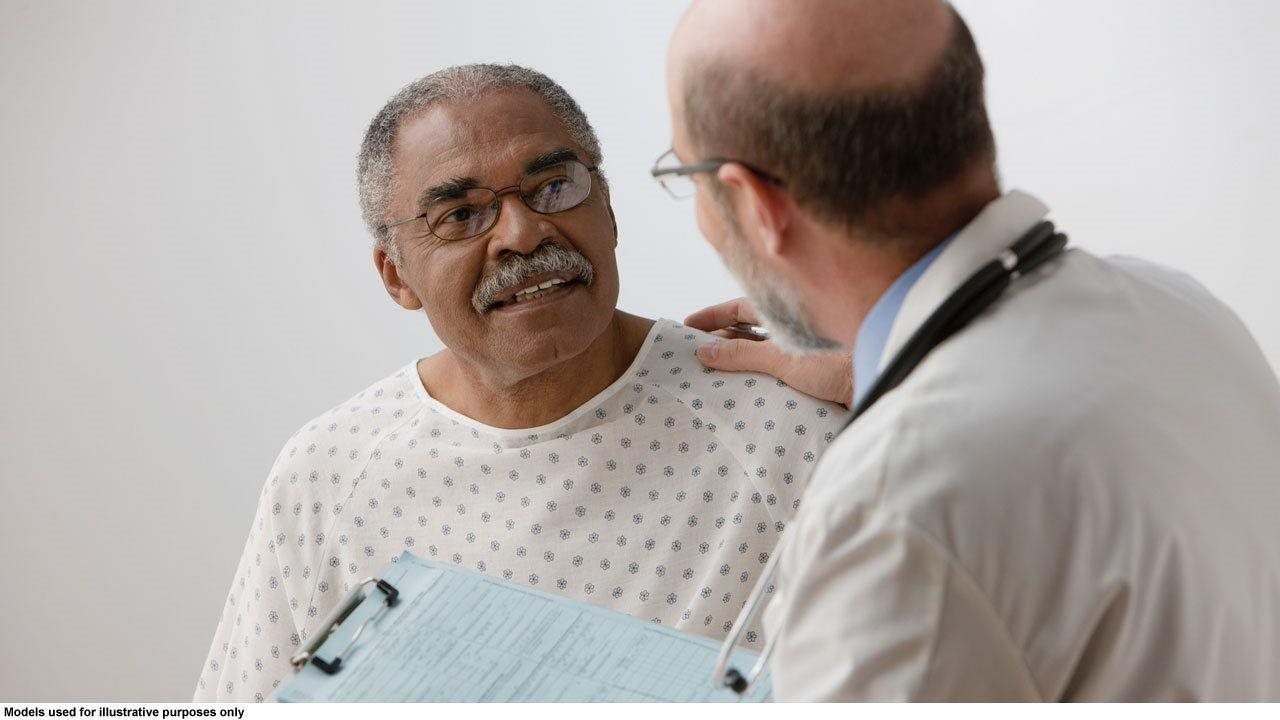
To help people, especially those over 65, stay heart healthy, Dr. Manesh Patel,* a Cardiologist at the Duke Heart Center in Durham, North Carolina, answers the most common questions about CAD.2
Q&A with Dr. Manesh Patel
Q: What is coronary artery disease – CAD – and how could it impact someone’s life?
A: In simple terms, CAD is the narrowing of blood vessels, also known as coronary arteries, that supply oxygen and blood to the heart.1 This is the most common type of heart disease and its complications are the leading cause of death for males and females in the U.S.1 CAD is very serious because patients with the condition are at a higher risk for health issues caused by blood clots such as stroke, heart attack, and cardiovascular-related death.1,3 That is why it’s so important for people to talk to their doctor or cardiologist about CAD and develop a treatment plan, if necessary.
CAD affects about 20.5 million Americans.4
Q: How does someone know if they have CAD?
A: Many patients come into my office with chest pain or discomfort, weakness, light-headedness, nausea, and shortness of breath, which are common symptoms of CAD.1 Pain or discomfort in the arms, neck, back, or shoulders can also be signs of CAD.1
I also consider other factors such as age, sex (men are generally at a higher risk of CAD), family history, smoking, high blood pressure, high blood cholesterol levels, diabetes, obesity, physical inactivity, stress, and eating an unhealthy diet because they can make someone have a higher risk for CAD.1 It’s always important to discuss any symptoms you have with your doctor or cardiologist because these are only some of the symptoms associated with CAD.1 Sometimes CAD can develop without any risk factors, or if you have multiple risk factors, you may be at even higher risk of developing CAD.5
After I evaluate my patients’ symptoms and discuss their medical history, I typically order lab tests to confirm a diagnosis.1 Other doctors and cardiologists may take a similar approach.
Q: Are there treatments to prevent the effects of CAD?
A: Yes, there are different ways to treat CAD. One medicine approved to prevent blood clots that are associated with CAD and other cardiovascular conditions is rivaroxaban (XARELTO®). When taken with aspirin, it can reduce the risk of major cardiovascular events, which is defined as cardiovascular death, heart attack, and stroke.6 XARELTO® may cause serious side effects including bleeding, which can be serious. It is important to talk to your doctor before beginning or stopping XARELTO®. Please see Important Safety Information below.
When considering the best treatment option for my patients, I often look at the latest clinical practice guidelines issued by reputable cardiology organizations. Guideline updates are important milestones that help keep healthcare providers up to date on the latest medicines and research to provide guidance on how to treat patients.
In July 2023, the American College of Cardiology (ACC) and the American Heart Association (AHA) updated their clinical practice guidelines for the management of chronic coronary disease, including CAD. The updated guidelines state that it is reasonable to use rivaroxaban (XARELTO®) plus an aspirin treatment regimen for patients at high ischemic risk and low bleeding risk to help reduce the risk of major cardiovascular events in patients with chronic coronary disease, otherwise known as CAD.7
XARELTO® (2.5 mg twice daily plus aspirin 75 mg-100 mg once daily) is the only approved direct oral anticoagulant drug in its class for the treatment of CAD.6 That said, it’s important to talk with your doctor or cardiologist to find the most appropriate treatment plan for you, as XARELTO® is not right for everyone.
Q: What should I ask my doctor about treating CAD?
A: If you think you or a loved one may have CAD, are experiencing any of the common signs and symptoms, or have any of the risk factors for the disease, it’s important to talk with your doctor or cardiologist. They will evaluate your symptoms and risk factors, and if you are diagnosed with CAD, develop a treatment plan that could include medication, exercise, and lifestyle changes.
It is important that CAD is diagnosed as soon as possible to help reduce the risk of serious outcomes such as heart attack and stroke.3
Questions to consider asking at your next doctor’s visit:
- My family has a history of heart disease. Does this increase my risk of CAD?
- I often feel short of breath. Could this be a sign that I have CAD?
- I have other health conditions. Might they be linked to CAD?
- I have CAD, what are my treatment options to help me manage my condition?
Finding the right CAD care is key to your overall heart health. If you or a loved one are experiencing symptoms of the disease, it is important to talk to your doctor. CAD is a serious condition but there is hope for people who may be at risk. You can learn more about CAD and how XARELTO® can help manage your condition by visiting Xarelto.com
Sponsored by Janssen Pharmaceutical companies of Johnson & Johnson
* Manesh Patel, M.D. is a paid consultant for the Janssen Pharmaceutical companies of Johnson & Johnson.
References:
- “All About Coronary Artery Disease.” Pacific Heart, Lung & Blood Institute, 2020.
- Xia, T. L., Huang, F. Y., Li, Y. M., Chai, H., Huang, B. T., Ou, Y. W., Li, Q., Pu, X. B., Zuo, Z. L., Peng, Y., Chen, M., & Huang, D. J. (2018). The impact of age on the implementation of evidence-based medications in patients with coronary artery disease and its prognostic significance: a retrospective cohort study. BMC public health, 18(1), 150. https://doi.org/10.1186/s12889-018-5049-x.
- “Symptoms of Coronary Artery Disease.” VeryWell Health, 2021.
- “Heart Disease and Stroke Statistics—2023 Update: A Report From the American Heart Association.” AHA Journals, 2023. Accessed June 24, 2023. https://www.ahajournals.org/doi/10.1161/CIR.0000000000001123#d1e727
- “Coronary Artery Disease.” MayoClinic, 2019.
- XARELTO® (rivaroxaban) [Prescribing Information]. Titusville, NJ: Janssen Pharmaceuticals, Inc.
- Virani, S. Salim et al. 2023 AHA/ACC/ACCP/ASPC/NLA/PCNA Guideline for the Management of Patients with Chronic Coronary Disease. Journal of the American College of Cardiology 2023.
Important Safety Information
WHAT IS XARELTO® (rivaroxaban)?
XARELTO® is a prescription medicine used to:
- reduce the risk of stroke and blood clots in adults who have a medical condition called atrial fibrillation that is not caused by a heart valve problem. With atrial fibrillation, part of the heart does not beat the way it should. This can lead to the formation of blood clots, which can travel to the brain, causing a stroke, or to other parts of the body
- treat blood clots in the veins of your legs (deep vein thrombosis or DVT) or lungs (pulmonary embolism or PE)
- reduce the risk of blood clots from happening again in adults who continue to be at risk for DVT or PE after receiving treatment for blood clots for at least 6 months
- help prevent a blood clot in the legs and lungs of adults who have just had hip or knee replacement surgery
- help prevent blood clots in certain adults hospitalized for an acute illness and after discharge, who are at risk of getting blood clots because of the loss of or decreased ability to move around (mobility) and other risks for getting blood clots, and who do not have a high risk of bleeding
XARELTO® is used with low dose aspirin to:
- reduce the risk of serious heart problems, heart attack and stroke in adults with coronary artery disease (a condition where the blood supply to the heart is reduced or blocked)
- reduce the risk of a sudden decrease in blood flow to the legs, major amputation, serious heart problems or stroke in adults with peripheral artery disease (a condition where the blood flow to the legs is reduced) and includes adults who have recently had a procedure to improve blood flow to the legs
XARELTO® is used in children to:
- treat blood clots or reduce the risk of blood clots from happening again in children from birth to less than 18 years, after receiving at least 5 days of treatment with injectable or intravenous medicines used to treat blood clots
- help prevent blood clots in children 2 years and older with congenital heart disease after the Fontan procedure
XARELTO® was not studied and is not recommended in children less than 6 months of age who:
- were less than 37 weeks of growth (gestation) at birth
- had less than 10 days of oral feeding, or
- had a body weight of less than 5.7 pounds (2.6 kg)
WHAT IS THE MOST IMPORTANT INFORMATION I SHOULD KNOW ABOUT XARELTO®?
XARELTO® may cause serious side effects, including:
- Increased risk of blood clots if you stop taking XARELTO®. People with atrial fibrillation (an irregular heart beat) that is not caused by a heart valve problem (nonvalvular) are at an increased risk of forming a blood clot in the heart, which can travel to the brain, causing a stroke, or to other parts of the body. XARELTO® lowers your chance of having a stroke by helping to prevent clots from forming. If you stop taking XARELTO®, you may have increased risk of forming a clot in your blood.
Do not stop taking XARELTO® without talking to the doctor who prescribes it for you. Stopping XARELTO® increases your risk of having a stroke. If you have to stop taking XARELTO®, your doctor may prescribe another blood thinner medicine to prevent a blood clot from forming.
- Increased risk of bleeding. XARELTO® can cause bleeding which can be serious and may lead to death. This is because XARELTO® is a blood thinner medicine (anticoagulant) that lowers blood clotting. During treatment with XARELTO® you are likely to bruise more easily, and it may take longer for bleeding to stop. You may be at higher risk of bleeding if you take XARELTO® and have certain other medical problems.
You may have a higher risk of bleeding if you take XARELTO® and take other medicines that increase your risk of bleeding, including:
-
- Aspirin or aspirin-containing products
- Long-term (chronic) use of non-steroidal anti-inflammatory drugs (NSAIDs)
- Warfarin sodium (Coumadin®, Jantoven®)
- Any medicine that contains heparin
- Clopidogrel (Plavix®)
- Selective serotonin reuptake inhibitors (SSRIs) or serotonin norepinephrine reuptake inhibitors (SNRIs)
- Other medicines to prevent or treat blood clots
Tell your doctor if you take any of these medicines. Ask your doctor or pharmacist if you are not sure if your medicine is one listed above.
Call your doctor or get medical help right away if you or your child develop any of these signs or symptoms of bleeding:
-
- Unexpected bleeding or bleeding that lasts a long time, such as:
- Nosebleeds that happen often
- Unusual bleeding from gums
- Menstrual bleeding that is heavier than normal, or vaginal bleeding
-
- Bleeding that is severe or you cannot control
- Red, pink, or brown urine
- Bright red or black stools (looks like tar)
- Cough up blood or blood clots
- Vomit blood or your vomit looks like “coffee grounds”
- Headaches, feeling dizzy or weak
- Pain, swelling, or new drainage at wound sites
- Spinal or epidural blood clots (hematoma). People who take a blood thinner medicine (anticoagulant) like XARELTO®, and have medicine injected into their spinal and epidural area, or have a spinal puncture, have a risk of forming a blood clot that can cause long-term or permanent loss of the ability to move (paralysis). Your risk of developing a spinal or epidural blood clot is higher if:
-
- A thin tube called an epidural catheter is placed in your back to give you certain medicine
- You take NSAIDs or a medicine to prevent blood from clotting
- You have a history of difficult or repeated epidural or spinal punctures
- You have a history of problems with your spine or have had surgery on your spine
If you take XARELTO® and receive spinal anesthesia or have a spinal puncture, your doctor should watch you closely for symptoms of spinal or epidural blood clots.
Tell your doctor right away if you have:
-
- back pain
- tingling
- numbness
- muscle weakness (especially in your legs and feet)
- or loss of control of the bowels or bladder (incontinence)
XARELTO® is not for use in people with artificial heart valves.
XARELTO® is not for use in people with antiphospholipid syndrome (APS), especially with positive triple antibody testing.
Do not take XARELTO® if you or your child:
- Currently have certain types of abnormal bleeding. Talk to your doctor before taking XARELTO® if you currently have unusual bleeding.
- Are allergic to rivaroxaban or any of the ingredients of XARELTO®.
Before taking XARELTO®, tell your doctor about all your medical conditions, including if you or your child:
- Have ever had bleeding problems
- Have liver or kidney problems
- Have antiphospholipid syndrome (APS)
- Are pregnant or plan to become pregnant. It is not known if XARELTO® will harm your unborn baby.
-
- Tell your doctor right away if you become pregnant during treatment with XARELTO®. Taking XARELTO® while you are pregnant may increase the risk of bleeding in you or in your unborn baby.
- Females who are able to become pregnant: Talk with your doctor about pregnancy planning during treatment with XARELTO®. Talk with your doctor about your risk for severe uterine bleeding if you are treated with blood thinner medicines, including XARELTO®.
- If you take XARELTO® during pregnancy, tell your doctor right away if you have any signs or symptoms of bleeding or blood loss. See “What is the most important information I should know about XARELTO®?” for signs and symptoms of bleeding.
- Are breastfeeding or plan to breastfeed. XARELTO® may pass into your breast milk. Talk to your doctor about the best way to feed your baby during treatment with XARELTO®.
Tell all of your doctors and dentists that you or your child are taking XARELTO®. They should talk to the doctor who prescribed XARELTO® for you before you have any surgery, medical or dental procedure.
Tell your doctor about all the medicines you or your child take, including prescription and over-the-counter medicines, vitamins, and herbal supplements.
Some of your other medicines may affect the way XARELTO® works, causing side effects. Certain medicines may increase your risk of bleeding. See “What is the most important information I should know about XARELTO®?”
HOW SHOULD I TAKE XARELTO®?
- Take XARELTO® exactly as prescribed by your doctor.
- Do not change your dose or stop taking XARELTO® unless your doctor tells you to. Your doctor may change your dose if needed.
- Your doctor will decide how long you should take XARELTO®.
- XARELTO® may need to be stopped for one or more days before any surgery or medical or dental procedure. Your doctor will tell you when to stop taking XARELTO® and when to start taking XARELTO® again after your surgery or procedure.
- If you need to stop taking XARELTO® for any reason, talk to the doctor who prescribed XARELTO® to you to find out when you should stop taking it. Do not stop taking XARELTO® without first talking to the doctor who prescribes it to you.
- If you have difficulty swallowing XARELTO® tablets whole, talk to your doctor about other ways to take XARELTO®.
- Do not run out of XARELTO®. Refill your prescription of XARELTO® before you run out. When leaving the hospital following a hip or knee replacement, be sure that you will have XARELTO® available to avoid missing any doses.
- If you take too much XARELTO®, go to the nearest hospital emergency room or call your doctor right away.
If you take XARELTO® for:
- Atrial Fibrillation that is not caused by a heart valve problem:
-
- Take XARELTO® 1 time a day with your evening meal.
- If you miss a dose of XARELTO®, take it as soon as you remember on the same day. Take your next dose at your regularly scheduled time.
- Blood clots in the veins of your legs or lungs:
-
- Take XARELTO® 1 or 2 times a day as prescribed by your doctor.
- For the 10-mg dose, XARELTO® may be taken with or without food.
- For the 15-mg and 20-mg doses, take XARELTO® with food at the same time each day.
- If you miss a dose:
- If you take the 15-mg dose of XARELTO® 2 times a day (a total of 30 mg of XARELTO® in 1 day): Take XARELTO® as soon as you remember on the same day. You may take 2 doses at the same time to make up for the missed dose. Take your next dose at your regularly scheduled time.
- If you take XARELTO® 1 time a day: Take XARELTO® as soon as you remember on the same day. Take your next dose at your regularly scheduled time.
- Hip or knee replacement surgery:
-
- Take XARELTO® 1 time a day with or without food.
- If you miss a dose of XARELTO®, take it as soon as you remember on the same day. Take your next dose at your regularly scheduled time.
- Blood clots in people hospitalized for an acute illness:
-
- Take XARELTO® 1 time a day, with or without food, while you are in the hospital and after you are discharged as prescribed by your doctor.
- If you miss a dose of XARELTO®, take it as soon as you remember on the same day. Take your next dose at your regularly scheduled time.
- Reducing the risk of serious heart problems, heart attack and stroke in coronary artery disease:
-
- Take XARELTO® 2.5 mg 2 times a day with or without food.
- If you miss a dose of XARELTO®, take your next dose at your regularly scheduled time.
- Take aspirin 75 to 100 mg once daily as instructed by your doctor.
- Reducing the risk of a sudden decrease in blood flow to the legs, major amputation, serious heart problems or stroke in people with peripheral artery disease, including those who have recently had a procedure to improve blood flow to the legs:
-
- Take XARELTO® 2.5 mg 2 times a day with or without food.
- If you miss a dose of XARELTO®, take your next dose at your regularly scheduled time.
- Take aspirin 75 to 100 mg once daily as instructed by your doctor.
For children who take XARELTO®:
- The dose of XARELTO® depends on your child’s body weight and will be calculated by your child’s doctor. Your child’s doctor will tell you if XARELTO® can be given to your child with or without food.
- The adult caregiver should give the dose.
- If your child is taking the tablet, the tablet should be taken whole and should not be split in an attempt to provide a lower dose of XARELTO®.
- If your child is taking the oral suspension, use the syringes provided in the original carton. The suspension will be prepared by the pharmacy. See the Instructions for Use included in the carton on how to properly give a dose of XARELTO® oral suspension to your child.
- Do not switch between the XARELTO® oral suspension or tablet without first talking to your doctor.
- If your child vomits or spits up:
-
- right after or within 30 minutes of taking the oral suspension, give a new full dose.
- more than 30 minutes after taking the oral suspension, do not give the dose again. Give the next dose at the regularly scheduled time.
- if vomiting or spitting up persists, contact your child’s doctor right away.
- If your child misses a dose:
-
- If your child is taking XARELTO® 1 time a day, give the dose as soon as you remember on the same day. If this is not possible, skip this dose and give the next dose at the regularly scheduled time.
- If your child is taking XARELTO® 2 times a day, give the missed morning dose as soon as you remember. You may give the missed morning dose together with the evening dose. However, a missed evening dose can only be taken in the same evening.
- If your child is taking XARELTO® 3 times a day, skip the missed dose and give the next dose at the regularly scheduled time.
WHAT ARE THE POSSIBLE SIDE EFFECTS OF XARELTO®?
XARELTO® may cause serious side effects:
- See “What is the most important information I should know about XARELTO®?”
The most common side effect of XARELTO® in adults was bleeding.
The most common side effects of XARELTO® in children include:
- bleeding
- vomiting
- cough
- inflamed stomach and gut
Call your doctor for medical advice about side effects. You may report side effects to FDA at 1-800-FDA-1088. You may also report side effects to Janssen Pharmaceuticals, Inc., at 1-800-JANSSEN (1-800-526-7736).
Please read full Prescribing Information, including Boxed Warnings, and Medication Guide for XARELTO®.
Trademarks are those of their respective owners.
cp-53637v8
cp-400546v1 01/24